
Every year, more than 795,000 American adults suffer a stroke, and one in four adults worldwide will suffer a stroke in their lifetime. Early action can reduce rates of death and disability.
Now, a group of Husker researchers, led by Steven Barlow, has patented a groundbreaking frontline treatment — the pTACS Somatosensory Biomedical Device — for cerebrovascular accidents that is portable, making it a versatile product for use in rehabilitation clinics, emergency rooms and, potentially, transport ambulances.
“It's a very low-cost device,” said Barlow, Corwin Moore Professor in special education and communication disorders, affiliate faculty in biological systems engineering and resident faculty in the Center for Brain, Biology and Behavior. “That means centers and rehabilitation facilities all over the country and beyond will be able to use this technology. Stroke is the number one health problem worldwide, now surpassing other types of diseases.”
The device includes a “smart” pneumatic controller and a microprocessor that is packaged inside a small black toolbox case and runs on rechargeable lithium-ion batteries — the same type and size of battery in a smartphone. The pTACS is a more compact, portable and precise successor to the Galileo, which Barlow’s team developed more than a decade ago to research how somatosensory treatment employing micro pulses of air could aid in stroke therapy. With funding from the National Institutes of Health, American Heart Association, Barkley Trust and Nebraska Research, Barlow was able to develop and fine-tune the somatosensory therapy protocols through individualized research trials at the University of Nebraska–Lincoln.
The success of those clinical trials led Barlow and team member Jacob Greenwood, a doctoral candidate in biomedical engineering, to focus the design of the device on performance, portability and usability. Barlow and Greenwood share inventor status on the U.S. patent.

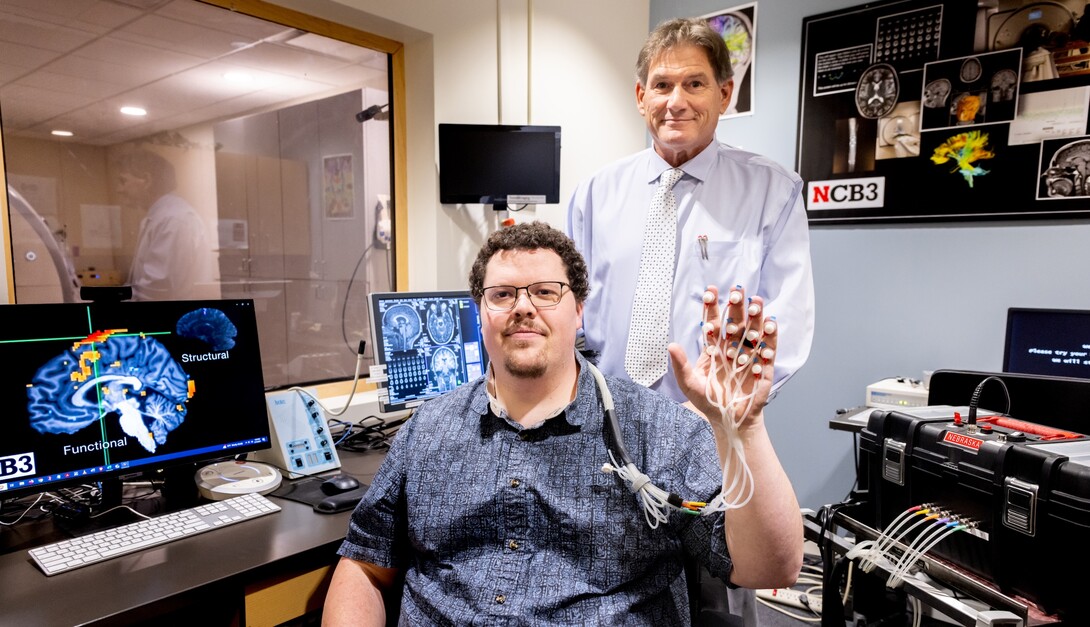
The pTACS biomedical device is a non-invasive method of brain stimulation. It utilizes rapidly compressed air pulses that are delivered through small plastic tubes into thermoplastic tactile "touch" capsules adhered to the hands, face, feet or other area of the skin to evoke repeated volleys of nerve responses. The pTACS stimulation has been shown to increase blood flow in tissues of the cerebral cortex that are near the damaged area of the brain. Animal models developed in the Frostig laboratory at the University of California, Irvine (Lay, Davis, Chen-Bee, Frostig, 2010) have shown that repeated somatosensory stimulation delivered during critical periods of recovery has the potential to save brain cells from death, preventing the formation of cerebral infarct.
“We take advantage of the inherent anatomy of the human brain — the way these sensory pathways are laid out — and by placing these cells on different parts of the body, we can selectively drive different parts of the brain with tremendous precision,” Barlow said.
The toolbox containing the pTACS hardware and firmware is attached to a small laptop containing the software to run the machine, delivering a programmed set of air pulses based on research Barlow and his students have conducted in the Barkley Speech-Language and Hearing Clinic and the Center for Brain, Biology and Behavior, and at other area institutions.
“The connected computer allows the user to select the protocol you want to run, and once that protocol is selected, it does everything,” Greenwood said.
Receiving a patent for the pTACS is a step in the process of getting FDA approval for the device. Barlow said he expects to receive an additional patent for his stroke treatment protocol and is working with NUtech Ventures to create a biomedical startup to manufacture and commercialize the device. Barlow has previous success with developing and commercializing groundbreaking medical devices. He developed and commercialized the NTrainer System 2.0, now sold and marketed internationally by Cardinal Health as the Kangaroo NTrainer System.
Frontline stroke treatment could be just one of the pTACS’ therapeutic possibilities. Barlow and his team are developing and seeking funding to further research treatment protocols for post-stroke injury and speech-language therapy functions, including for those on the autism spectrum disorder.
“We’ve had some patients in the clinic, and they're at least six months post injury. Some of them are two and three years after their stroke, and we're still able to generate very significant improvements in their function,” Barlow said. “This therapy could be administered by a speech-language pathologist, physical therapist, nurse practitioner or someone with a neuroscience background.
“In a current MRI study in collaboration with UNO Department of Biomechanics (Dr. Mukul Mukherjee) and UNMC Department of Neurology (Dr. Pierre Fayad), we use the pTACS device to drive mechanosensory nerve endings in the feet to stimulate the balance and gait system and activate related brain pathways.”
Barlow anticipates more therapeutic uses for the pTACS device will be uncovered through additional research.
“It's got a really good trajectory,” he said. “And we have a vibrant team. We have a lot of investigators, and many students interested in this.”








